Are you wondering how to treat the burned roof of the mouth? Your external skin is not the only portion of your body that is more susceptible to getting burned. Gulping a sizeable hot pizza slice can burn the hard palate of your mouth, commonly known as the roof of the mouth.
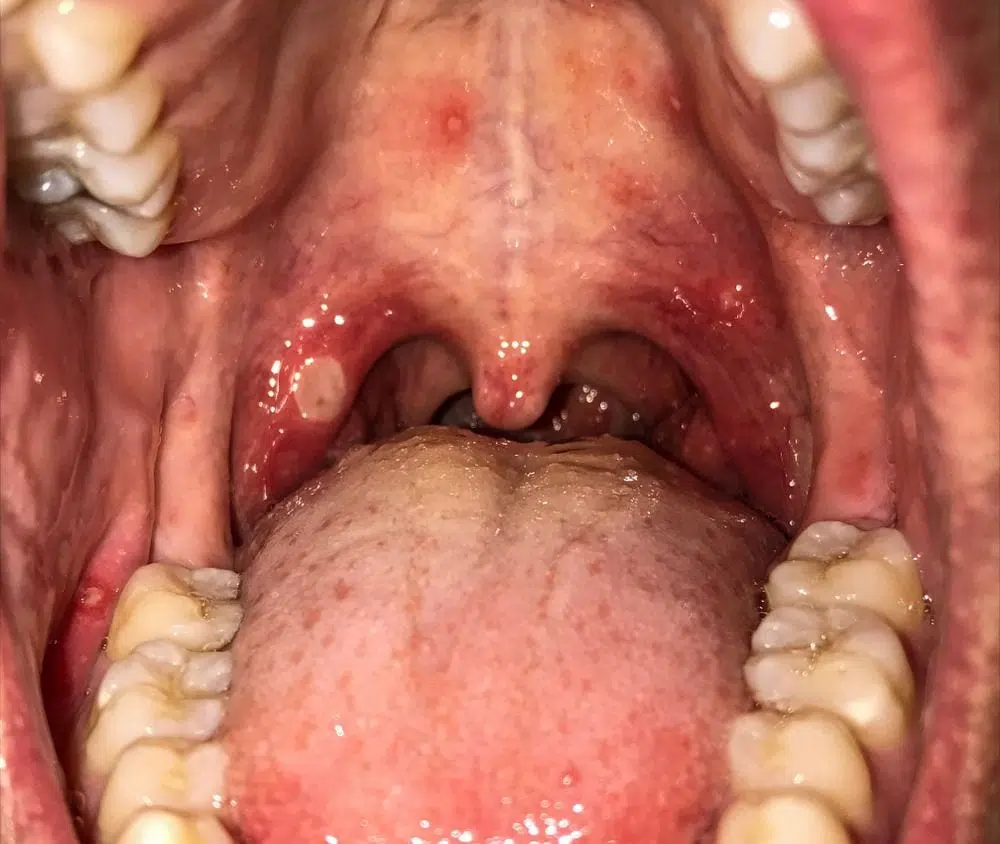 You might have come across many food items by which you burned the roof of your mouths, such as hot coffee, hot tea, or a hot slice of pizza. A bite into fresh food from the oven can also burn your tongue. Our mouth has numerous soft tissues that are sensitive to hot drinks and food. Even if we try to control the urge, we still end up eating hot food and burning the roof of our mouths. The tissues of our hard palate are highly susceptible to burns compared to other soft tissues in the body as they are notably more delicate and thinner. To appreciate the sensations of drinking and eating, this skin on the roof of the mouth is fragile, and thus, it can be damaged easily. Learning how to treat the burned roof of the moth is highly useful if you are fond of eating fresh, hot food from the oven. Here’s how to treat burned roof f the mouth easily using specific simple home remedies.
You might have come across many food items by which you burned the roof of your mouths, such as hot coffee, hot tea, or a hot slice of pizza. A bite into fresh food from the oven can also burn your tongue. Our mouth has numerous soft tissues that are sensitive to hot drinks and food. Even if we try to control the urge, we still end up eating hot food and burning the roof of our mouths. The tissues of our hard palate are highly susceptible to burns compared to other soft tissues in the body as they are notably more delicate and thinner. To appreciate the sensations of drinking and eating, this skin on the roof of the mouth is fragile, and thus, it can be damaged easily. Learning how to treat the burned roof of the moth is highly useful if you are fond of eating fresh, hot food from the oven. Here’s how to treat burned roof f the mouth easily using specific simple home remedies.
How To Treat The Burned Roof Of The Mouth
First-degree burns, also known as minor burns on the roof of the mouth, do not necessarily need medical attention. Managing most minor burns in the mouth is quite simple. Here are a few common approaches you can use at home to treat minor burns:
1. How To Treat The Burned Roof Of The Mouth Using Food And Drink
As soon as you feel the burn, try something frozen or cool, such as ice, to relieve the pain. A few drinks, such as milk, usually coat the roof of the mouth. They present a layer that gives relief that water cannot. Some food items that may help are:
- sugarless gum
- soft, creamy food items such as yogurt, cheeses, sour cream, and ice creams.
- Frozen or cold foods such as ice pops, applesauce, and pudding.
When you are healing from the burned roof within your mouth, avoid eating crunchy foods or some foods that have sharp ends or edges. Such foods may worsen the skin of the mouth. Do not consume hot or spicy foods, too. Try eating cool, soft foods till the mouth burns completely heal.
2. How To Treat The Burned Roof Of The Mouth Using Mouth Rinses
Infections after a minor mouth burn occurs are highly rare. You can perform saltwater rinses that help deal with mouth pain and have been bestowed to improve wound healing. Make the rinse at home by dissolving half a teaspoon of salt into 8 ounces of lukewarm water. You must arrange salt and lukewarm water solution three to four times a day for relief.
3. How To Treat The Burned Roof Of The Mouth Using Over-the-counter Medications
You can also start taking an over-the-counter (OTC) medication to help reduce the pain and swelling resulting from mouth burns. Common Over-The-Counter medicines for pain relief include acetaminophen or Tylenol, ibuprofen or Advil, benzocaine, or Orajel. Do not consume more than the prescribed dosage daily of each of the given medications.
4. How To Treat The Burned Roof Of The Mouth Using Aloe vera
Aloe vera can also alleviate pain from a skin burn, and you can take it orally as well. Search for mouth rinses that have aloe vera essence inside of them, and you will get such rinses online or nearest stores. You can also obtain aloe vera in gel form and juice form. Currently, no studies are found that demonstrate aloe vera’s application in the healing of mouth burns. Due to its remarkable properties, it is considered to be helpful.
5. What To Avoid
Your mouth ordinarily heals entirely in about a week or so. To promote speed up the treatment process, here are a few valuable tips that might help:
- Do not eat acidic foods and drinks such as coffee, orange juice, and tomatoes.
- Do not eat spicy foods.
- Do not consume products having mint and cinnamon (try shifting to flavor-free toothpaste).
- Do not intake alcohol or tobacco products.
How to find out mouth burns are severe.
First-degree wounds or burns are known to cause minimal skin injury. They are also known as “superficial burns” as they only attack the outermost covering of the skin. Symptoms of a first-degree burn might include these:
- redness
- Insignificant inflammation or swelling
- Discomfort and pain.
- Dry and peeling skin that is seen as soon as the burn heals
A further severe burn, like a second-degree or third-degree burn, needs urgent medical attention and treatment. A few symptoms of these burns can include the following:
- Sharp pain
- blistering
- redness
- swelling
Not only blisters, but you might also mark pockets of pus if further infection occurs in the roof of your mouth. A third-degree burn will also affect the nerves in the mouth, and other structures get damaged. The impaired nerves by burns might not be capable of relaying pain signals to the brain. These kinds of burns may cause dangerous complications.
Burning Mouth Syndrome
You might sense a burning sensation in the roof of your mouth, and it might not have any apparent cause. If such pain continues to trouble you for days or weeks at a time, you might be having burning mouth syndrome or BMS. A few common signs referring to Burning Mouth Syndrome include:
- Scalding or burning pain in the mouth for no apparent reason.
- numbness inside the mouth
- Occurrence of dry mouth
- Bitter, metallic, or other strange tastes inside the mouth
- pain or numbness in the tongue, lips, or gums
Burning Mouth Syndrome makes you feel as if you have scalded or burned the mouth’s tissues, but there are no apparent changes to your skin. It could be mild or painful like you have eaten something scorching. But Burning Mouth Syndrome is usually not predictable and can happen without prior warning. It might last for a few days or get over without stopping, or it might appear once or twice every few weeks or months. Burning Mouth Syndrome is of two types. Basic BMS is not prompted due to another medical ailment and might result from nerve pathways when they are damaged. Secondary BMS occurs as a result of another medical condition such as:
- Diabetes
- trauma
- acid reflux
- cancer therapy
- mouth infection
- Vitamin deficiency
- Thyroid issues
If you feel burning sensations inside your mouth for a prolonged time, discuss with your doctor to examine you for Burning Mouth Syndrome. It might be hard to diagnose. The doctor might practice several specific tests to determine, including blood tests, saliva tests, tissue biopsies, or allergy tests. Treating BMS conditions depends on the root cause. There is no cure for BMS, but the doctor might suggest any of the following treatments:
- lidocaine medicine or another topical remedy
- Clonazepam (anticonvulsant)
- oral medicines for nerve pain relief
- Cognitive-behavioral therapy to relieve the pain
The doctor might also suggest taking added dietary supplements to heal the root cause of the burning pain. If you possess dentures, the doctor might suggest you replace them.
When to visit the doctor
In a few instances, the mouth burn might grow so painful that none of these home remedies would give any relief. You might have a severe burn if you notice:
- white patches or sores appear within your mouth
- you acquire a fever
- the burn is not healing quickly as it should
- you have issues while swallowing food.
Ask for medical treatment if you mark burns with any of the mentioned symptoms. Burns might need an in-office visit or emergency room treatment, based on its severity. Second-degree burns need a medical procedure to treat them. However, you might be able to relieve the pain using some OTC medications like acetaminophen or ibuprofen. Third-degree burns require emergency treatment. When in uncertainty, talk to your doctor or visit a critical care center. Explain to your doctor the symptoms, other treatment options you have already tried, and how well the treatments have worked. You and the doctor can work toegther to determine the most suitable course of treatment for your present condition of mouth burns. If you sense a severe burn, you might need antibiotics to combat bacterial germs in the mouth. Some well-known antibiotics used are ampicillin, oxacillin, amoxicillin/clavulanate, cefazolin, and penicillin. If there is critical damage to your oral cavity or nearby structures, the doctor might require to execute a skin graft surgery or other types of surgeries to store function to that portion again.
How to handle mouth burns in children
If your child receives a first-degree burn in the mouth after eating something hot, manage the burn in a similar way like you would do for an adult. Begin first by giving them milk to drink or other frozen or cold drinks. If your child senses much pain and discomfort, provide them with relevant doses of medications like acetaminophen and ibuprofen. Do not use any medications that have components that your child might be allergic to. Also, practice benzocaine sparingly because it has been known to cause rare but severe risks and side effects. The skin might peel for the coming two to three days before it begins to heal, and it might lead to causing your child more pain and discomfort. If these symptoms do not get better after two or three days, visit a good child doctor. If unusual fluids or pus begins to leak from the mouth burn or your child catches a fever, talk to the healthcare provider right away. If your child acquires a second- or third-degree burn, head to the doctor immediately for prompt treatment and a complete evaluation of your child. The doctor might also assess if further damage to the nerves or some other problems to determine.
The Bottom Line
Maximum cases of first-degree mouth burns can be treated easily at home using remedies and go away on their own in a matter of a few days. Critical mouth burns may require long-term medications to protect skin tissue and help the nerves within your mouth heal fully. See the doctor if you consider the burns are critical. Getting the proper treatment at the right time is necessary to prevent permanent damage, scar formation, diseases, and other complications.
References:
- https://www.newhealthguide.org/Roof-Of-Mouth-Hurts.html
- https://www.mayoclinic.org/diseases-conditions/burning-mouth-syndrome/symptoms-causes/syc-20350911
- https://www.mayoclinic.org/first-aid/first-aid-burns/basics/art-20056649
- https://unmhealth.org/
